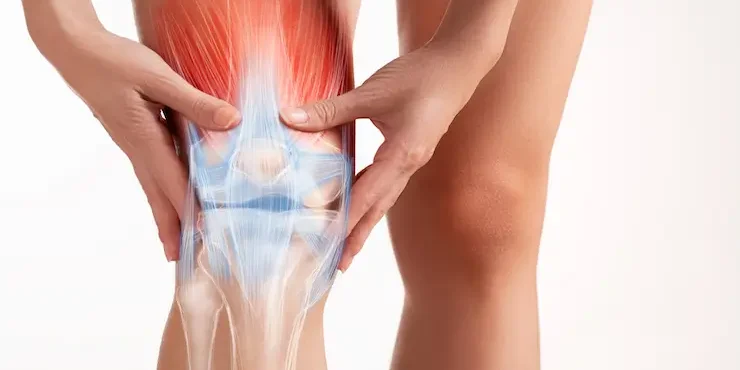
Testing For Osteoarthritis
Osteoarthritis is a common degenerative joint disease that affects millions of people worldwide, causing pain, stiffness, and reduced mobility. Early detection and accurate diagnosis are crucial for managing symptoms and preventing further joint damage. If you suspect you have osteoarthritis, understanding the various testing methods can help you take the necessary steps to confirm the diagnosis and begin appropriate treatment. In this article, we will explore the common tests and procedures used to diagnose osteoarthritis.
What Is Osteoarthritis?
Osteoarthritis is a type of arthritis characterized by the breakdown of cartilage—the protective tissue that cushions the ends of the bones in your joints. As the cartilage wears away, bones can rub against each other, causing pain, swelling, and decreased joint mobility. Over time, osteoarthritis can lead to the development of bone spurs and other changes in the joint structure. Learn more about osteoarthritis and its impact on joint health.
Common Symptoms of Osteoarthritis
Before testing for osteoarthritis, it’s essential to recognize the common symptoms associated with the condition. These may include:
- Joint Pain: Persistent or intermittent pain in the affected joint, particularly after activity or towards the end of the day.
- Stiffness: Joint stiffness, especially in the morning or after periods of inactivity.
- Swelling: Swelling around the joint, which may be accompanied by tenderness.
- Reduced Range of Motion: Difficulty moving the joint through its full range of motion.
- Grating Sensation: A feeling of grating or grinding when moving the joint.
Diagnostic Tests for Osteoarthritis
To diagnose osteoarthritis, healthcare providers use a combination of patient history, physical examination, and imaging tests. Here are the most common methods used to test for osteoarthritis:
1. Medical History and Physical Examination
The first step in diagnosing osteoarthritis involves taking a detailed medical history and performing a physical examination. Your healthcare provider will ask about your symptoms, when they started, and how they have progressed over time. They will also inquire about any previous injuries, family history of arthritis, and other medical conditions that could contribute to joint pain.
During the physical examination, the provider will assess the affected joints for signs of osteoarthritis, such as swelling, tenderness, and decreased range of motion. They may also check for the presence of bone spurs or other structural changes.
2. X-Rays
X-rays are one of the most common imaging tests used to diagnose osteoarthritis. X-rays can reveal:
- Joint Space Narrowing: As cartilage wears away, the space between the bones in the joint becomes narrower, a hallmark sign of osteoarthritis.
- Bone Spurs: X-rays can show the presence of bone spurs (osteophytes), which are bony growths that develop along the edges of bones in response to joint damage.
- Bone Changes: In advanced cases of osteoarthritis, X-rays may reveal changes in bone structure, such as increased bone density (subchondral sclerosis) or the development of bone cysts.
Learn more about how X-rays are used in the diagnosis of osteoarthritis.
3. Magnetic Resonance Imaging (MRI)
While X-rays are useful for visualizing bone changes, they do not provide detailed images of soft tissues such as cartilage, tendons, and ligaments. In some cases, your healthcare provider may recommend an MRI to get a more detailed view of the joint.
MRI scans use powerful magnets and radio waves to create detailed images of the joint’s internal structures. This can help detect early signs of cartilage damage, inflammation, and other soft tissue changes that may not be visible on X-rays.
4. Blood Tests
While there is no specific blood test to diagnose osteoarthritis, blood tests may be used to rule out other types of arthritis that can cause similar symptoms, such as rheumatoid arthritis or gout. Common blood tests include:
- Rheumatoid Factor (RF) Test: Used to check for the presence of rheumatoid factor, an antibody often found in people with rheumatoid arthritis.
- Erythrocyte Sedimentation Rate (ESR) and C-Reactive Protein (CRP) Tests: These tests measure levels of inflammation in the body, which can help differentiate osteoarthritis from inflammatory forms of arthritis.
Learn more about the role of blood tests in diagnosing different types of arthritis.
5. Joint Aspiration (Arthrocentesis)
In some cases, your healthcare provider may perform a procedure called joint aspiration or arthrocentesis to analyze the fluid inside the affected joint. During this procedure, a needle is inserted into the joint space to withdraw a small sample of synovial fluid. The fluid is then examined for signs of inflammation, infection, or the presence of crystals, which can help distinguish osteoarthritis from other joint conditions like gout or septic arthritis.
Conclusion
Testing for osteoarthritis involves a combination of medical history, physical examination, imaging tests, and, in some cases, laboratory tests. Early diagnosis is key to managing symptoms and preventing further joint damage. If you are experiencing joint pain, stiffness, or other symptoms of osteoarthritis, it’s important to consult with a healthcare provider who can guide you through the appropriate tests and develop a personalized treatment plan.
Your doctor can often diagnose osteoarthritis based on your age, your typical symptoms, and examination of your affected joints. Tests such as X-rays or blood tests are usually not necessary. However, sometimes your doctor may suggest X-rays or other tests if they are uncertain about the diagnosis and want to exclude other problems. Call Advanced Health Solutions – GA Spine & Disc, today at (770) 926-9495 we offer high-quality, effective, and safe osteoarthritis treatment Woodstock.